Drop in adult flu vaccinations may be factor in last season’s record-breaking deaths, illnesses10/26/2018
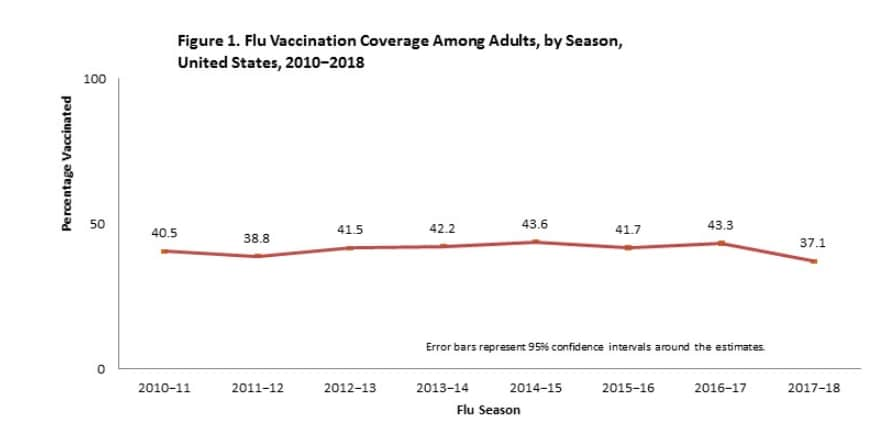
Editor's Note: What if it's all these vaccinations over the decades that's making people more susceptible to the flu virus? Fewer than 4 out of 10 adults in the United States got flu shots last winter, the lowest rate in seven seasons and one likely reason that the 2017-2018 season was the deadliest in decades. Reports released Thursday by the Centers for Disease Control and Prevention provide new details outlining the severity of the past flu season, during which more people were killed by seasonal influenza than in any other since the 1970s. Flu vaccination is the main way to prevent sickness and death caused by flu. But last season, vaccination coverage among adults was 37.1 percent, a decrease of 6.2 percentage points from the previous season. That’s the lowest rate for adults 18 and older since 2010-2011. For many years, overall vaccination coverage has remained flat, with less than half of the U.S. population getting vaccinated. But the most recent drop has caused concern among experts. “That’s huge. It’s a striking inflection down from the previous year,” said William Schaffner, an infectious-diseases expert at Vanderbilt University and medical director of the National Foundation for Infectious Diseases. Data released Thursday also provide a comprehensive picture of the impact of last season’s deadly respiratory virus. Some data about deaths and hospitalizations were released last month, but new details show the scope of last season’s harshness. The CDC estimates that:
Last winter’s flu season was so devastating for several reasons. It was dominated by an especially fierce virus strain. Seasons where H3N2 is dominant typically result in the most complications, especially for the very young and the old, experts say. Vaccines are also less effective against H3N2. The virus changes rapidly, requiring more updates to the seasonal vaccine, and making it that much harder for the body’s immune system to generate a good response. The drop in vaccine coverage also could have contributed to last season’s severity, said Alicia Fry, chief of epidemiology and prevention in CDC’s influenza division. Flu vaccine, while far from perfect, reduces illness and serious complications, such as hospitalizations and admission to intensive-care units. Schaffner and CDC officials said the drop in vaccine coverage could be related to preliminary reports about low vaccine effectiveness in Australia. Flu activity in the southern hemisphere can often predict what Americans might expect. “I think that really discouraged a lot of people from getting vaccinated,” said Schaffner, who noted that the early data about the vaccine’s effectiveness in Australia was incorrect. It’s too early to know whether people are “still carrying that around in their minds,” he said. It’s still unclear what this coming flu season will be like. Flu activity is low, but there has already been one child death reported. Last season, the flu killed 183 children, the most since federal health authorities began tracking pediatric deaths 14 years ago. About 80 percent of those children were unvaccinated. It takes about two weeks after getting a flu shot for the body to generate a full immune response. “This is the perfect time,” said the CDC’s Fry, noting that flu activity is still relatively low. This year, CDC officials are hoping to boost vaccine coverage by helping doctors and nurses make a strong case to their patients for a flu shot. A strong recommendation from a clinician makes a huge difference in whether someone gets the influenza vaccine. This year, the CDC has created new tools for clinicians, including videos, on making a strong flu vaccine recommendation, said Cindy Weinbaum, deputy director of CDC’s immunization services division. That includes identifying and addressing any questions or concerns in plain and understandable language. Ahead of the brunt of this winter’s flu season, the Food and Drug Administration on Wednesday approved the first new type of flu drug in two decades. Xofluza is a pill for people age 12 and older. It can reduce the severity and shorten the duration of flu symptoms after one dose, FDA officials said. But to get the most benefits, the medicine needs to be taken within 48 hours of becoming sick with flu symptoms. The drug works by slowing down the replication of the virus in the body. So the earlier a person can take the medicine, the sooner it can catch the infection and the better it works. “If you start it later, you already have a ton of virus wreaking havoc,” said the CDC’s Fry, who welcomed more options for health-care providers. The drug was developed by the Roche Group and Shionogi & Co. During last winter’s severe flu season, there was a shortage of the anti-viral medicine Tamiflu and other generic anti-viral drugs. By Lena H. Sun October 25 at 12:57 PM https://www.washingtonpost.com/health/2018/10/25/drop-adult-flu-vaccinations-may-be-factor-last-seasons-record-breaking-deaths-illnesses/
Comments are closed.
|
Archives
March 2021
|
 RSS Feed
RSS Feed